Overview
The article focuses on the significance of the A1C test and its relationship to blood sugar management for individuals with diabetes, emphasizing how the A1C to blood sugar chart aids in diagnosis and treatment. It supports this by detailing the A1C percentage ranges that indicate normal, prediabetic, and diabetic conditions, and underscores the importance of lifestyle changes, regular monitoring, and collaboration with healthcare professionals to effectively manage blood sugar levels and improve overall health outcomes.
Introduction
In a world where diabetes affects millions, understanding the A1C test becomes essential for effective health management. This vital blood test measures average blood sugar levels over the past few months, serving as a cornerstone for diagnosing type 2 diabetes and guiding treatment strategies. With clear benchmarks indicating normal, prediabetic, and diabetic ranges, the A1C test empowers individuals to take charge of their health.
As diabetes prevalence continues to rise, particularly among younger populations, the importance of early diagnosis and proactive management cannot be overstated. This article delves into the significance of the A1C test, offers insights into interpreting results, and provides actionable strategies for maintaining healthy levels through lifestyle changes and regular monitoring. Understanding the nuances of A1C can lead to better health outcomes and a more informed approach to diabetes care.
What is the A1C Test and Why is it Important?
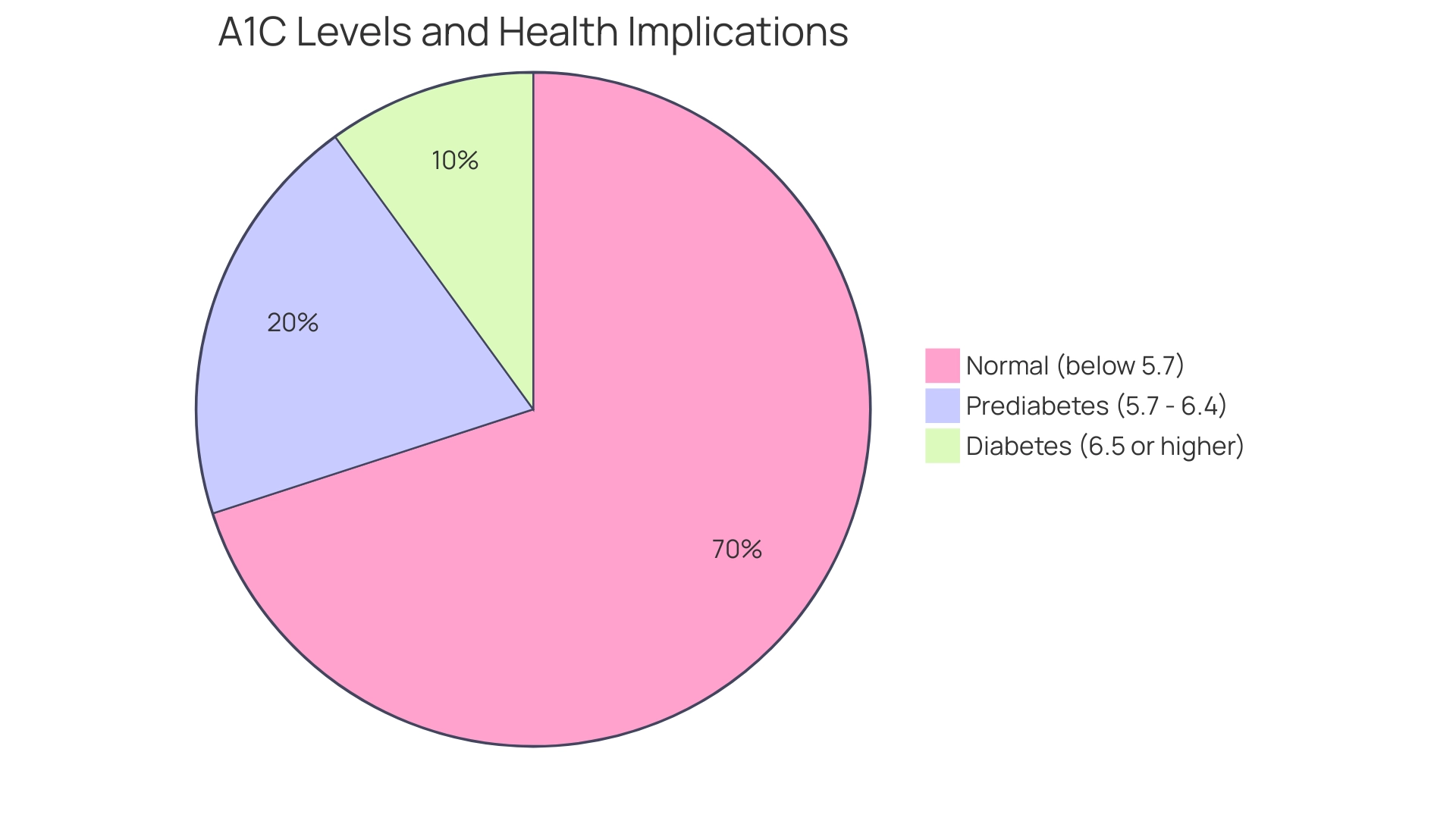
The A1C test acts as an essential indicator of your average blood sugar amounts over the past two to three months, which is crucial for the A1C to blood sugar chart used in diagnosing type 2 diabetes and assessing blood sugar control. According to the A1C to blood sugar chart:
- A measurement below 5.7% is considered normal.
- Values ranging from 5.7% to 6.4% suggest prediabetes.
- A threshold of 6.5% or higher on the A1C to blood sugar chart verifies a diagnosis of diabetes, highlighting the test’s significance in directing effective treatment strategies.
To improve your A1C readings and overall health, consider adopting a holistic lifestyle approach suited for San Marcos, CA. This includes:
- Focusing on a balanced diet rich in fresh, local produce from vibrant farmers’ markets, such as avocados, berries, and leafy greens.
- Incorporating regular outdoor exercise at scenic parks and trails like Lake San Marcos and Discovery Lake.
- Engaging with community wellness programs for additional support.
As noted by experts, the A1C to blood sugar chart is a valuable tool for managing blood sugar disorders and other glycemic control issues, but it functions best in an interprofessional healthcare team environment to be effective.
Collaborating with healthcare professionals, including personalized guidance from experts like Dr. Jason Shumard, can empower you to integrate these essential lifestyle changes effectively. The urgency of effective management of this condition is underscored by the fact that in 2021, it was linked to 399,401 death certificates, emphasizing the need for proactive strategies to maintain healthy A1C levels. Grasping the nuances of the A1C test in relation to the A1C to blood sugar chart can empower patients to make informed decisions regarding their health and treatment plans, ensuring a proactive approach to managing their condition.
Furthermore, the rising incidence of type 1 diabetes among children and adolescents underscores the importance of early diagnosis and management, making access to resources crucial for effective diabetes care.
Understanding the Connection Between A1C Levels and Blood Sugar
A1C values, indicated as a percentage, act as a vital sign of average glucose management over a prolonged duration. For instance, an A1C of 6% relates to an average glucose concentration of roughly 126 mg/dL, demonstrating the direct connection shown in the a1c to blood sugar chart between A1C percentages and glucose concentrations. Higher A1C values, as shown on the a1c to blood sugar chart, reflect poorer blood sugar management, emphasizing the importance of monitoring these levels.
Understanding this relationship empowers type 2 patients to recognize how daily choices—such as diet, exercise, and medication adherence—impact their long-term health outcomes and overall well-being. Effective strategies, like implementing SMART goals for regular glucose monitoring and utilizing tracking methods such as fitness apps and journals, can significantly enhance management of the condition. Engaging in programs like Dr. Jason Shumard’s 30-Day Diabetes Reset has proven transformative for many patients.
Recent research indicates that A1C levels may not effectively identify individuals with intermediate hyperglycemia or undiagnosed conditions, highlighting the need for comprehensive monitoring. Moreover, statistics indicate that from 2012 to 2022, excess medical costs per individual related to this condition rose from $10,179 to $12,022, underscoring the financial implications of managing this health issue. Insights from specialists in glucose management, including Nathan, emphasize that their success is attributable to the number of CGM glucose measurements (8000) performed in the month prior to HbA1c measurement.
Achieving lower A1C percentages can significantly improve health outcomes, making it essential for patients to consistently track their glucose metrics using an A1C to blood sugar chart, regularly review their progress, and adapt their goals accordingly. Research indicates that goal-setting persistence scores can positively impact performance, with scores improving from 3.4 (SD = 2.0) to 3.8 (SD = 1.9) in specific conditions, demonstrating the effectiveness of structured goal-setting.
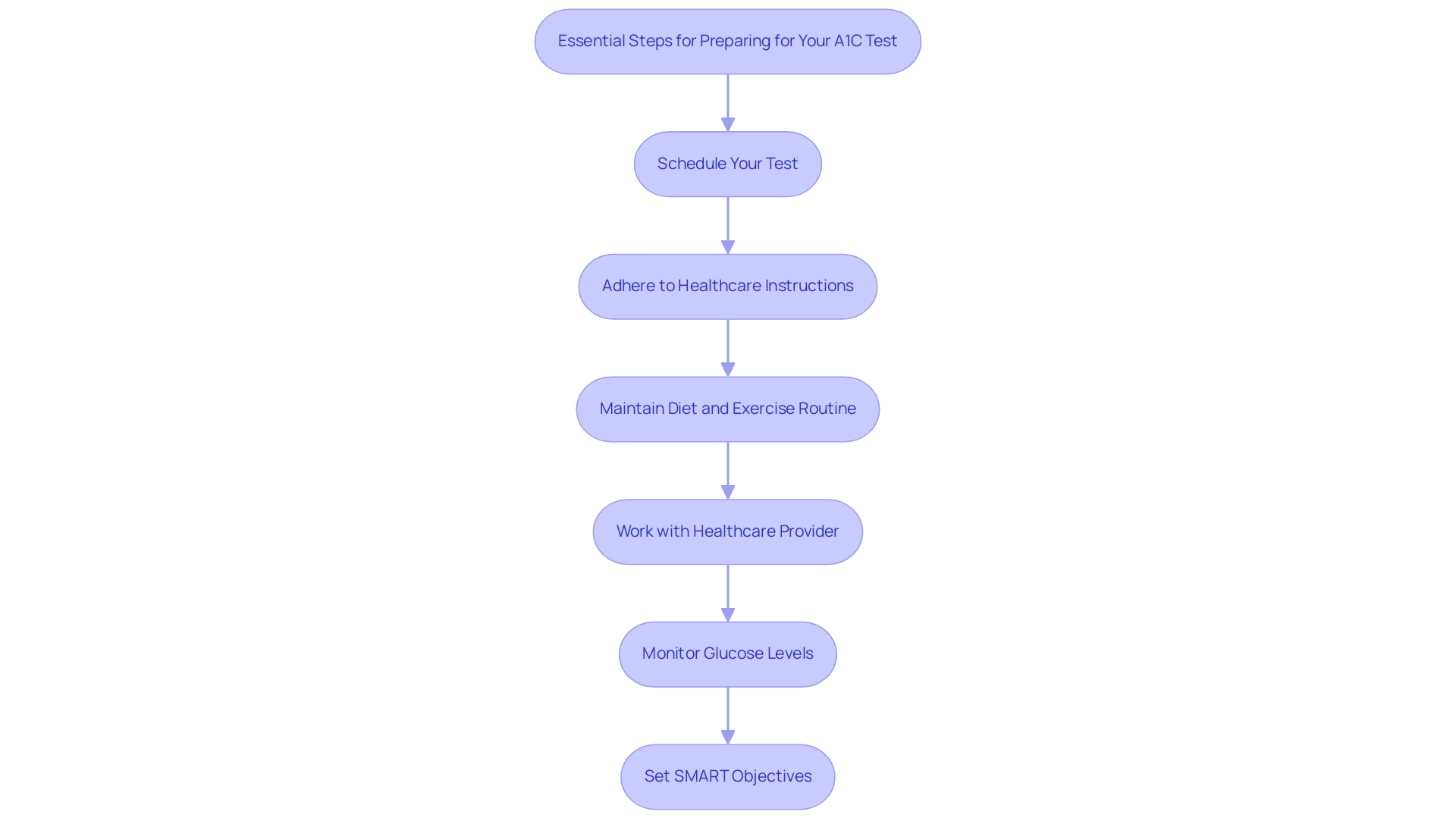
Preparing for Your A1C Test: Essential Steps
Preparing for your A1C test is crucial for accurate results, and there are several essential steps to consider:
-
Schedule your test at a time that allows you to maintain a consistent routine. This consistency is vital, as fluctuations in your daily activities can affect your results.
The ARIC study found that 60% of participants with fasting glucose ≥126 mg/dl at baseline also had fasting glucose ≥126 mg/dl at the 3-year follow-up visit, highlighting the importance of consistent testing conditions.
-
Adhere to any specific instructions provided by your healthcare provider, which may include fasting if required. Proper adherence to these guidelines is key to obtaining an accurate A1C result.
Additionally, measuring plasma insulin and proinsulin concentrations is necessary for diagnosing non-diabetes-related hypoglycemia, further emphasizing the need for accurate testing and preparation.
-
Avoid making significant changes to your diet or exercise routine leading up to the test. Such changes can introduce variability, potentially skewing your results.
Instead, think about utilizing this time to monitor your food consumption and activity amounts through fitness applications, journals, or even pedometers, in accordance with effective progress tracking methods.
An expert in managing blood sugar levels once stated,
Hemoglobin A1C is a valuable tool in handling diabetes mellitus and other glycemic control disorders, but it is most effective when used in conjunction with an a1c to blood sugar chart within an interprofessional healthcare team environment.
This highlights the importance of working closely with your healthcare team to ensure that your preparation is aligned with best practices. For instance, working together with your healthcare provider can assist you in identifying the optimal time to arrange your test and any required dietary modifications.
Moreover, continuous research indicates that early identification and regular tracking of glucose measurements can greatly influence results, as observed in instances of gestational diabetes mellitus (GDM). Women diagnosed with GDM early are more likely to experience adverse outcomes, reinforcing the need for effective preparation for A1C testing. Establishing SMART objectives—specific, measurable, attainable, relevant, and time-bound—can also assist in regulating glucose concentrations effectively.
Additionally, it is crucial to set appropriately challenging goals, as research indicates that there can be systematic negative relationships between goal achievement and goal difficulty. By adhering to these guidelines, you can improve the likelihood that your A1C results will accurately represent your sugar management on the a1c to blood sugar chart, enhancing your overall health outcomes.
Interpreting Your A1C Results: What Do the Numbers Mean?
The A1C results, displayed as a percentage, reflect an individual’s average blood glucose readings over the past two to three months, as shown in the a1c to blood sugar chart. According to the A1C to blood sugar chart:
- A level below 5.7% is regarded as normal.
- Levels between 5.7% and 6.4% suggest prediabetes.
- An A1C of 6.5% or above confirms a diagnosis of the condition.
Engaging in a detailed discussion with your healthcare provider is crucial to understanding how these results relate to your overall health and wellness.
For individuals already diagnosed with this condition, frequent A1C testing serves as an essential tool for monitoring progress on the a1c to blood sugar chart toward achieving personalized health goals. This proactive approach enables timely adjustments to treatment plans, ensuring optimal glycemic control. As emphasized by healthcare experts such as Roopa Naik, ‘Hemoglobin A1c is a valuable tool in managing metabolic disorders and other glycemic control issues, but it functions best in an interprofessional healthcare team environment to be effective.’
This emphasizes the significance of teamwork in managing diabetes-related health. Furthermore, in the scenic environment of San Marcos, CA, engaging in local wellness programs can enhance support systems, offering personalized guidance from experts like Dr. Jason Shumard. The community also provides resources for healthy eating, including vibrant farmers’ markets, where you can find fresh, local produce that contributes to a diabetes-friendly diet.
Additionally, it’s important to consider the financial implications of managing this condition, as excess medical costs per person have increased significantly, highlighting the need for comprehensive support in managing these expenses. The prevalence of diabetes is closely linked to weight status, emphasizing the need for obesity management in prevention efforts. By integrating lifestyle changes with the a1c to blood sugar chart, individuals can achieve better health outcomes and enhance their overall quality of life.
Effective Strategies for Lowering A1C Levels Naturally
-
Adopt a Balanced Diet: Emphasizing a diet rich in whole foods is essential for managing A1C values effectively. Tailored nutrition strategies, like those provided in functional medicine, can encompass personalized meal plans aimed at stabilizing glucose amounts and enhancing metabolic function. Incorporate a variety of fresh, local fruits, vegetables, lean proteins, and whole grains while minimizing processed foods and sugars.
Research indicates that dietary quality plays a crucial role in blood glucose management; individuals with higher genetic risk for type 2 conditions may experience even greater benefits from maintaining a healthy, nutrient-dense diet. A study found that a higher DRV score (per two-point increase) was inversely associated with %HbA1c by − 0.023% (or 0.23 mmol/mol), indicating the importance of tailored dietary recommendations that can significantly lower A1C levels and improve overall health. Given that diabetes prevalence is predicted to rise from 425 million people in 2017 to 629 million by 2045, effective management strategies are more crucial than ever.
-
Increase Physical Activity: Engaging in regular physical activity is vital for sugar control. Aim for at least 150 minutes of moderate aerobic exercise per week. Such activities can lead to substantial improvements in A1C measurements, which can be tracked on an a1c to blood sugar chart, as consistent exercise promotes better glycemic responses and overall metabolic health.
-
Monitor Your Glucose: Keeping track of your sugar amounts is crucial to understanding how different foods and activities affect your measurements on the a1c to blood sugar chart. Regular monitoring allows for personalized changes to your diet and exercise routine, leading to an accurate a1c to blood sugar chart and more effective glucose management. Continuous glucose monitoring has proven particularly useful in assessing glycemic responses to dietary changes, providing valuable insights for patients.
-
Stay Hydrated: Sufficient hydration is frequently neglected but is essential for managing sugar concentrations. Consuming ample water can aid in sustaining optimal hydration, which is advantageous for overall metabolic functioning and can help in managing A1C values. Consider local beverage options in San Marcos, such as herbal teas or infused water, which can provide hydration without added sugars.
-
Manage Stress: Ongoing stress can adversely affect glucose readings, making stress management techniques essential. Incorporating methods like mindfulness, yoga, or deep breathing exercises can significantly assist in stabilizing blood glucose. By addressing stress through natural strategies, individuals can improve their A1C management and overall well-being.
The Importance of Regular A1C Monitoring and Follow-Up
Efficient management of blood sugar relies on the regular examination of A1C readings, which can be tracked using the a1c to blood sugar chart, usually suggested every three to six months. An A1C level of 6.5% or higher signifies the condition, emphasizing the importance of using an A1C to blood sugar chart not only for monitoring but also for diagnosing the ailment. This routine assessment is crucial for you and your healthcare provider to evaluate the efficacy of your current treatment plan and make informed adjustments as needed.
Regular A1C monitoring helps in identifying trends in sugar control and is essential for understanding the a1c to blood sugar chart, empowering you to take proactive steps to reduce the risk of complications. Additionally, Continuous Glucose Monitoring (CGM) technology has rapidly evolved, providing valuable data that complements A1C measurements and enhances management of the condition. It’s crucial to recognize that A1C results may also be conveyed as estimated Average Glucose (eAG) and can be understood using an a1c to blood sugar chart, which can vary from home glucose meter readings; comprehending these distinctions is essential for effective management of health.
According to the American Diabetes Association, the preprandial glycemic target has shifted from 70–130 mg/dL to 80–130 mg/dL, illustrating the importance of keeping abreast of updated care standards. Engaging in follow-up discussions with your healthcare team about your results fosters a collaborative approach to your health management, underscoring the significance of being an active participant in your diabetes care journey. Furthermore, embracing holistic lifestyle strategies—such as regular outdoor exercise in the scenic parks of San Marcos and a balanced diet featuring local produce—can profoundly impact your health outcomes.
Utilizing various tracking methods, including fitness apps, journals, and pedometers, can enhance your ability to monitor progress and set SMART goals. Research indicates that goal-setting persistence scores can significantly improve performance, and by understanding your A1C trends and utilizing an a1c to blood sugar chart along with community support, you can make informed decisions that enhance not only your blood sugar control but also your overall well-being.
Conclusion
Understanding the A1C test is paramount for anyone navigating the complexities of diabetes management. This vital blood test not only serves as a diagnostic tool for type 2 diabetes but also provides critical insights into long-term blood sugar control. With clearly defined benchmarks, individuals can better understand their health status and make informed decisions regarding their lifestyle and treatment plans.
Regular monitoring of A1C levels, coupled with proactive engagement in healthy practices—such as balanced nutrition, consistent physical activity, and stress management—can significantly improve health outcomes. The correlation between A1C percentages and average blood sugar levels highlights the importance of daily choices and underscores the need for a comprehensive approach to diabetes care that includes collaboration with healthcare professionals.
Moreover, the rising incidence of diabetes, particularly among younger demographics, emphasizes the urgency for early diagnosis and effective management strategies. By adopting a holistic perspective that incorporates community resources and support systems, individuals can empower themselves to maintain healthy A1C levels and improve their quality of life. Ultimately, understanding and leveraging the insights provided by the A1C test is a crucial step toward achieving better health outcomes and fostering a proactive approach to diabetes management.
Frequently Asked Questions
What does the A1C test measure?
The A1C test measures your average blood sugar levels over the past two to three months, which is crucial for diagnosing type 2 diabetes and assessing blood sugar control.
What are the classifications based on the A1C to blood sugar chart?
According to the A1C to blood sugar chart: 1. Below 5.7% is considered normal. 2. 5.7% to 6.4% indicates prediabetes. 3. 6.5% or higher confirms a diagnosis of diabetes.
How can individuals improve their A1C readings and overall health?
Individuals can improve their A1C readings by adopting a holistic lifestyle that includes: – A balanced diet rich in fresh, local produce. – Regular outdoor exercise. – Participation in community wellness programs.
Why is the A1C test important in diabetes management?
The A1C test is vital for managing blood sugar disorders and glycemic control issues. It is most effective when used in collaboration with an interprofessional healthcare team to direct treatment strategies.
What is the significance of collaborating with healthcare professionals regarding A1C management?
Collaborating with healthcare professionals provides personalized guidance, helping patients integrate essential lifestyle changes effectively for better management of their condition.
What recent statistics highlight the urgency of managing A1C levels?
In 2021, diabetes was linked to 399,401 death certificates, underscoring the need for proactive strategies to maintain healthy A1C levels.
How do A1C values relate to average glucose concentrations?
An A1C of 6% corresponds to an average glucose concentration of approximately 126 mg/dL, demonstrating the direct connection between A1C percentages and glucose concentrations.
What strategies can help in managing diabetes effectively?
Effective strategies include setting SMART goals for regular glucose monitoring and utilizing tracking methods like fitness apps and journals.
What does recent research suggest about A1C levels and undiagnosed conditions?
Recent research indicates that A1C levels may not effectively identify individuals with intermediate hyperglycemia or undiagnosed conditions, emphasizing the need for comprehensive monitoring.
How can tracking glucose metrics impact health outcomes for diabetes patients?
Consistently tracking glucose metrics using an A1C to blood sugar chart and regularly reviewing progress can significantly enhance the management of diabetes and improve health outcomes.