Overview
Managing type 2 diabetes can be challenging, but making the right food choices can truly make a difference. It’s important to recognize that incorporating low-glycemic index foods, such as:
- Non-starchy vegetables
- Whole grains
- Lean proteins
- Healthy fats
can significantly stabilize your blood sugar levels. On the other hand, it’s wise to avoid high-glycemic options like:
- Sugary beverages
- Refined carbohydrates
Many patients find that these dietary selections not only help with glucose regulation but also improve overall health. Research supports this, showing that low-GI diets lead to better weight management and glucose control. Remember, you’re not alone on this journey; making these changes can lead to a healthier, more balanced life. Consider exploring the 30-Day Diabetes Reset program to further support your efforts.
Introduction
Dietary choices play a crucial role in managing type 2 diabetes, affecting everything from glucose levels to overall well-being. It’s important to recognize that understanding the glycemic index of foods can empower you to make informed decisions that support stable energy and effective blood sugar control. Many individuals find themselves overwhelmed by the multitude of options available.
How can you navigate the best and worst food choices to optimize your health outcomes? This article delves into essential dietary selections, offering insights into the best foods to embrace and the pitfalls to avoid, ultimately guiding you toward a healthier lifestyle.
Understanding Food Choices for Type 2 Diabetes
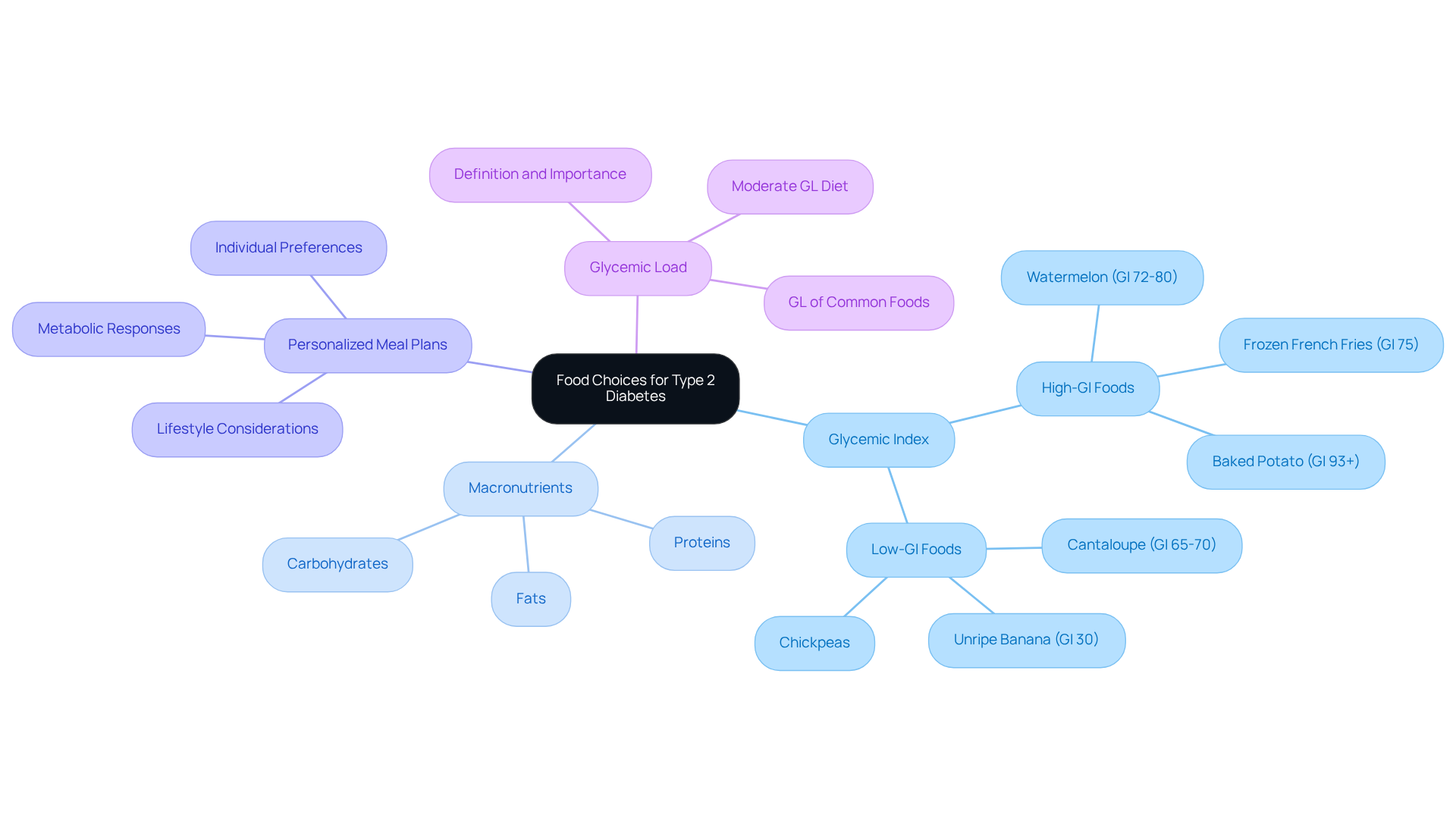
Dietary selections play a vital role in managing type 2 diabetes, profoundly affecting glucose levels and overall well-being. It’s important to recognize that understanding the glycemic index (GI) of foods can make a significant difference. High-GI choices may lead to quick spikes in blood sugar, while low-GI alternatives can help maintain steady energy levels. For example, watermelon has a high GI of 72 to 80, which can cause rapid increases in blood sugar. In contrast, options like cantaloupe, with a lower GI of about 65 to 70, can be more favorable for blood sugar management.
Many patients find that balancing macronutrients—carbohydrates, proteins, and fats—is crucial for how their bodies process nutrients. Incorporating fiber-rich foods, such as whole grains and legumes, can slow digestion and enhance glycemic control. Research shows that low-GI diets not only aid in managing blood sugar levels but also support weight loss and improved health outcomes. For instance, individuals following a low-GI diet often experience reduced hemoglobin A1C levels, which is essential for effective blood sugar management.
Nutritionists emphasize the importance of personalized meal plans that consider individual preferences, lifestyles, and metabolic responses to different foods. This tailored approach allows patients to manage their diabetes effectively while enjoying a variety of foods. By focusing on low-GI carbohydrates and maintaining a balanced intake of macronutrients, individuals can significantly improve their glucose management and overall well-being. Additionally, paying attention to glycemic load (GL), which averages under 80 grams per 2,000 calories, can further assist in regulating carbohydrate intake and stabilizing glucose levels.
Best Food Options for Managing Type 2 Diabetes
Managing type 2 diabetes can feel overwhelming at times, but making the right food type 2 diabetes choices can significantly ease this journey. Here are some optimal selections that can help you take control of your health:
-
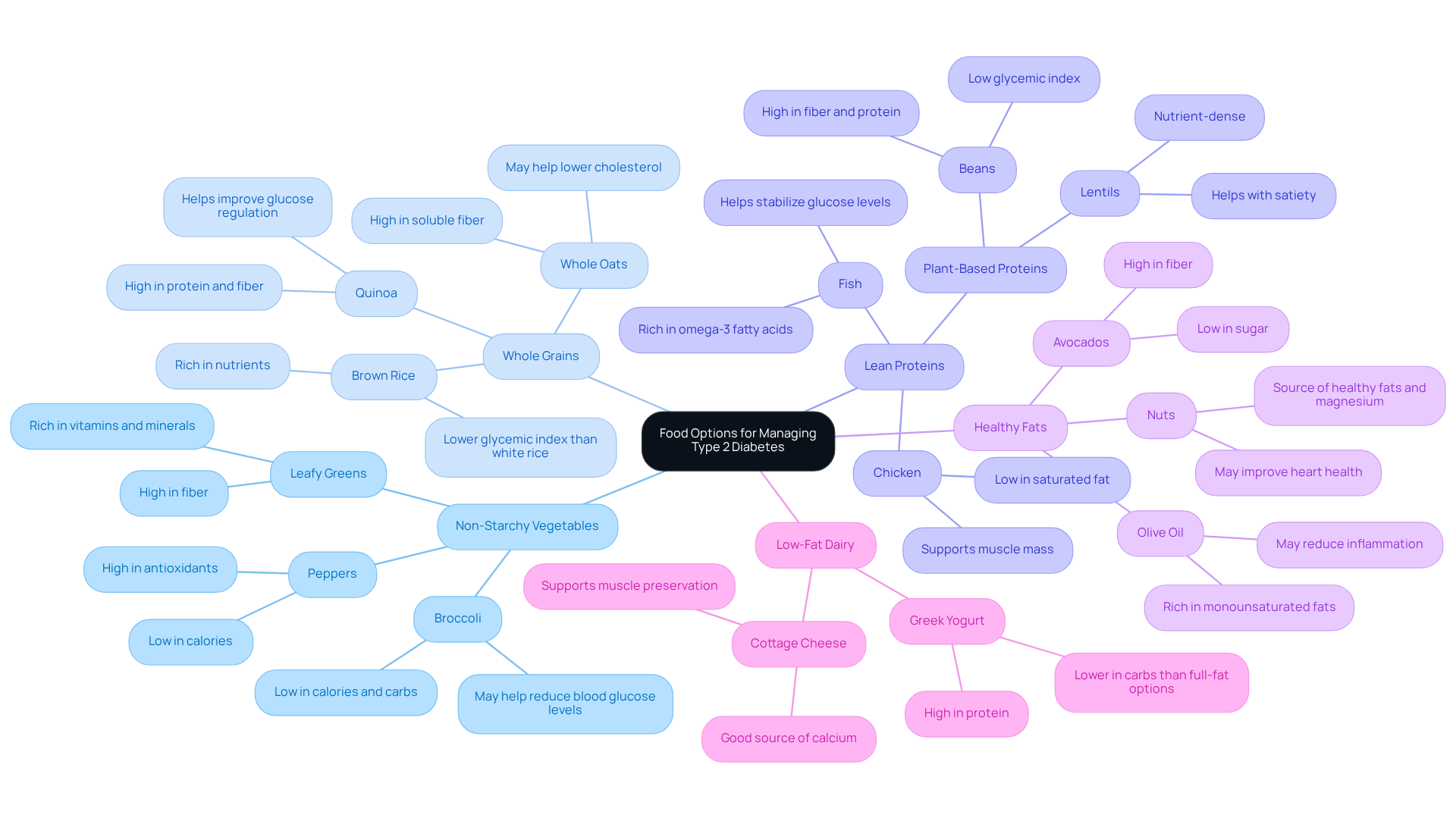
Non-starchy vegetables: Leafy greens, broccoli, and peppers are not only delicious but also low in calories and carbohydrates, making them fantastic allies for blood sugar control. Research shows that incorporating a variety of these vegetables can greatly enhance glycemic management. Aim to fill half your plate with non-starchy vegetables; it’s a simple way to support portion control and nourish your body.
-
Whole grains: Foods like quinoa, brown rice, and whole oats are packed with fiber and essential nutrients. They play a crucial role in improving glucose regulation. Studies indicate that those who opt for whole grains experience fewer glucose spikes compared to those who choose refined grains. The Dietary Guidelines for Americans suggest swapping at least half of your refined grains for whole grains, reinforcing their importance in a balanced diet.
-
Lean proteins: Including sources such as chicken, turkey, fish, and plant-based proteins like beans and lentils is vital for maintaining muscle mass and promoting satiety. These proteins help stabilize glucose levels and contribute to your overall well-being. It’s also beneficial to add a small serving of high-fiber carbohydrates at each meal to keep you feeling satisfied.
-
Healthy fats: Incorporating avocados, nuts, and olive oil into your meals can boost heart health while providing essential fatty acids without raising blood glucose levels. These fats are not only good for your metabolism but also help reduce inflammation, supporting your overall health.
-
Low-fat dairy: Options like Greek yogurt and cottage cheese offer protein and calcium with lower carbohydrate levels than full-fat varieties. Including these dairy products can help with muscle preservation and bone health while managing your carbohydrate intake.
It’s important to recognize that heavily processed items, refined grains, and sweetened drinks can hinder your efforts to maintain optimal glucose levels. By thoughtfully incorporating these dietary categories associated with food type 2 diabetes into your daily meals, you can achieve more stable glucose levels and enhance your overall health. Remember, you’re not alone in this journey, and small, manageable changes can lead to significant improvements.
Are you ready to take the next step toward a healthier you? Consider joining the 30-Day Diabetes Reset program for more guidance and support.
Worst Food Choices to Avoid with Type 2 Diabetes
For individuals managing food type 2 diabetes, it’s vital to be mindful of certain food choices to maintain stable blood sugar levels. Have you ever noticed how some foods can affect your energy throughout the day? It’s important to recognize that avoiding specific items can significantly improve your well-being.
-
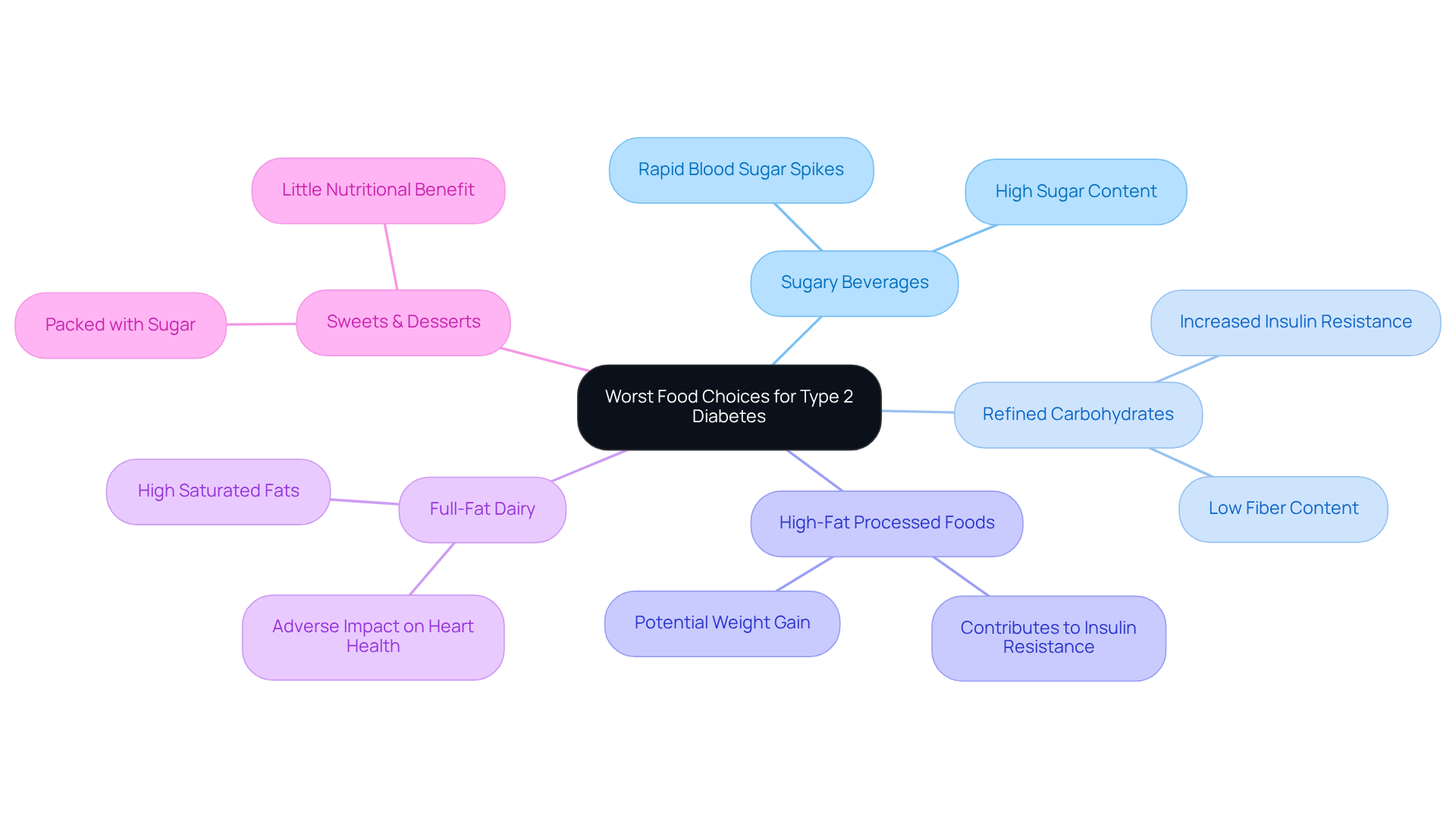
Sugary beverages: Drinks such as sodas, sweetened teas, and energy drinks can cause rapid spikes in blood sugar due to their high sugar content. Research suggests that these drinks can lead to considerable glucose variations, making them particularly challenging for blood sugar management. Carrie Madormo, RN, MPH, reminds us that uncontrolled intake of refined carbs can lead to health issues over time.
-
Refined carbohydrates: Foods like white bread, pastries, and many processed snacks are low in fiber, triggering quick increases in glucose levels. Many patients find that diets rich in refined carbohydrates are linked to heightened insulin resistance, which can complicate blood sugar management over time.
-
High-fat processed foods: Items such as fried foods and certain fast-food options contribute to insulin resistance and can lead to weight gain, further complicating blood sugar management. It’s essential to consider how these choices affect your health journey.
-
Full-fat dairy items: These items often contain high amounts of saturated fats, which can adversely impact heart health and insulin sensitivity. This presents additional risks for individuals facing blood sugar challenges.
-
Sweets and desserts: Cakes, cookies, and candies are usually packed with sugar and provide little nutritional benefit, making them unsuitable for managing glucose levels. Have you ever felt a sugar crash after indulging in sweets? It’s a common experience.
By steering clear of these items, individuals can enhance their glucose regulation and overall well-being when considering food type 2 diabetes. Dr. Shumard’s center emphasizes the importance of education and personalized care, providing valuable resources to help patients make informed dietary choices. Remember, you’re not alone on this journey; support is available to guide you toward healthier living.
Strategies for Making Healthy Food Choices
Making informed and healthy food choices can feel overwhelming at times, but there are several effective strategies that can help you navigate this journey with confidence:
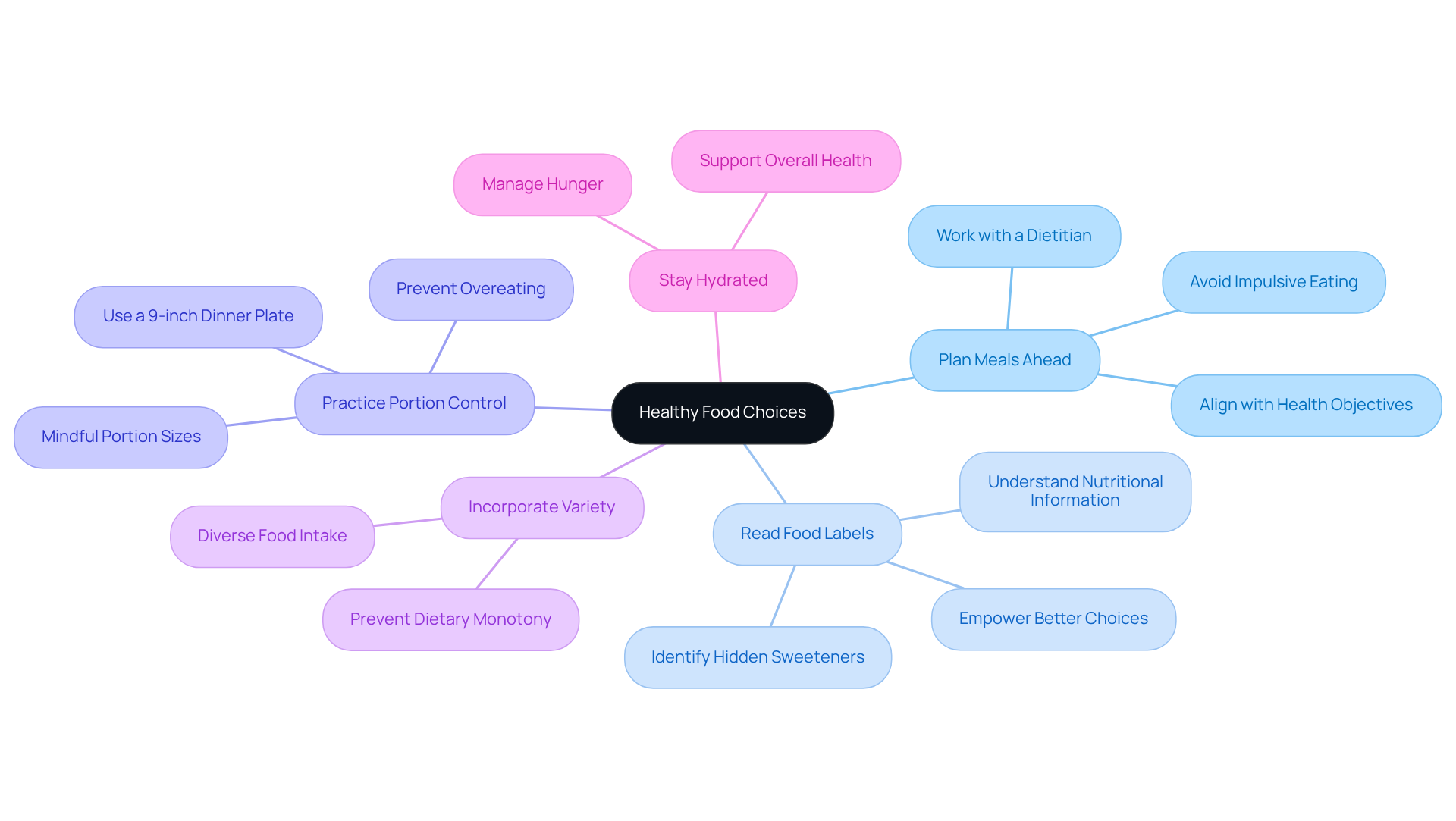
- Plan Meals Ahead: Preparing meals in advance not only helps you avoid impulsive eating but also ensures balanced nutrition, which is crucial for managing blood sugar levels. Many find that working with a dietitian or health educator can further customize meal plans to align with their personal health objectives.
- Read Food Labels: Understanding nutritional information—especially regarding sweeteners and carbohydrate content—empowers you to make better dietary choices. It’s encouraging to see that more diabetes patients are actively examining labels to avoid hidden sweeteners and unhealthy components, which plays a vital role in effective diabetes management.
- Practice Portion Control: Being mindful of portion sizes is essential for preventing overeating and maintaining stable blood sugar levels. For example, using a 9-inch dinner plate can help you balance meals effectively and prevent excessive calorie intake.
- Incorporate Variety: Eating a diverse range of foods ensures you receive a well-rounded intake of nutrients and helps prevent dietary monotony, which can lead to healthier eating habits.
- Stay Hydrated: Drinking plenty of water not only helps manage hunger but also supports your overall health, making it easier to stick to your dietary goals.
By applying these strategies, you can take control of your dietary choices, leading to better management of food type 2 diabetes and an improved quality of life. Dietitians emphasize that meal planning is a fundamental aspect of effective management, particularly for food type 2 diabetes, as it allows you to synchronize your food selections with your health objectives. With approximately 1 in 10 Americans living with diabetes, it’s clear how important these strategies are for everyone.
Conclusion
Dietary choices play a crucial role in managing type 2 diabetes, influencing blood sugar levels and overall health. It’s important to recognize that understanding the glycemic index (GI) of foods, along with a balanced intake of macronutrients, can empower individuals to make informed decisions that promote better glucose control. By prioritizing low-GI foods and incorporating a variety of nutrient-dense options, individuals can effectively support their health while enjoying a diverse diet.
Many patients find that implementing key strategies for managing type 2 diabetes through food choices can make a significant difference. Emphasizing the importance of:
- Non-starchy vegetables
- Whole grains
- Lean proteins
- Healthy fats
- Low-fat dairy
illustrates how these foods can stabilize glucose levels and enhance overall well-being. Conversely, it is crucial to be aware of the detrimental impact of:
- Sugary beverages
- Refined carbohydrates
- High-fat processed foods
- Full-fat dairy
- Sweets
which can disrupt blood sugar management. Implementing:
- Meal planning
- Reading food labels
- Practicing portion control
- Staying hydrated
are essential strategies that can facilitate healthier eating habits.
Ultimately, making mindful food choices is not just about managing diabetes; it is about embracing a lifestyle that fosters long-term health and well-being. As individuals navigate their dietary journeys, support and resources, such as personalized meal plans and educational programs, can significantly enhance their efforts. Taking proactive steps towards healthier eating can lead to improved health outcomes and a better quality of life for those living with type 2 diabetes. Remember, you’re not alone in this journey, and every small step counts towards a healthier future.
Frequently Asked Questions
Why is understanding food choices important for managing type 2 diabetes?
Dietary selections are crucial for managing type 2 diabetes as they significantly affect glucose levels and overall well-being.
What is the glycemic index (GI) and why does it matter?
The glycemic index (GI) measures how quickly foods raise blood sugar levels. High-GI foods can cause rapid spikes in blood sugar, while low-GI foods help maintain steady energy levels.
Can you provide examples of high-GI and low-GI foods?
Watermelon has a high GI of 72 to 80, which can rapidly increase blood sugar, whereas cantaloupe has a lower GI of about 65 to 70, making it more favorable for blood sugar management.
How do macronutrients affect diabetes management?
Balancing carbohydrates, proteins, and fats is crucial for how the body processes nutrients, which can impact blood sugar levels.
What role do fiber-rich foods play in managing type 2 diabetes?
Fiber-rich foods, such as whole grains and legumes, can slow digestion and enhance glycemic control, aiding in better blood sugar management.
What are the benefits of following a low-GI diet?
Low-GI diets can help manage blood sugar levels, support weight loss, and improve health outcomes, including reduced hemoglobin A1C levels.
Why is a personalized meal plan important for diabetes management?
Personalized meal plans consider individual preferences, lifestyles, and metabolic responses, allowing for effective diabetes management while enjoying a variety of foods.
How can glycemic load (GL) assist in regulating carbohydrate intake?
Monitoring glycemic load, which averages under 80 grams per 2,000 calories, can help stabilize glucose levels by regulating carbohydrate intake.