Introduction
The management of diabetes has evolved significantly, driven by advancements in education, technology, and personalized care strategies. Central to effective diabetes management is the understanding of self-care practices, which encompass:
- Monitoring blood glucose levels
- Adhering to medication regimens
- Making informed dietary choices
As the prevalence of type 2 diabetes continues to rise, particularly among younger populations, the necessity for comprehensive education and support becomes increasingly critical. This article explores various facets of diabetes management, highlighting the importance of:
- Lifestyle changes
- The role of healthcare professionals
- The impact of innovative technologies
By examining evidence-based strategies and real-life success stories, it aims to provide a thorough overview of how individuals can take charge of their health and improve their quality of life through informed decision-making and proactive management.
Foundations of Diabetes Management: Self-Care and Education
Effective diabetes management pdf starts with a thorough understanding of the condition and the critical importance of self-care. Self-care behaviors encompass a range of activities such as:
- Regularly monitoring blood glucose levels
- Adhering to prescribed medications
- Making informed dietary choices
Education is pivotal in this process, empowering individuals to understand their diabetes management pdf, recognize symptoms of both hyperglycemia and hypoglycemia, and implement necessary lifestyle adjustments.
Transformative wellness outcomes can be observed in success stories from Dr. Jason Shumard’s 30-Day Diabetes Reset Program, where individuals report significant improvements in their metrics, including substantial weight loss and reduced reliance on medications. For instance, one individual shared,
‘I have lost 55 lbs. My A1C started at 9.1 after 8 months it is now 5.7. Fasting glucose was at 133 and now it is at 85.’
Another noted,
‘I lost a lot of weight, have more energy and feel great. I am not depressed anymore and I don’t need my meds anymore!!!’
These testimonials highlight the program’s effectiveness in reversing type 2 conditions and enabling individuals to take control of their health. Recent statistics indicate that during a recent period, 5,293 children and adolescents aged 10 to 19 were diagnosed with type 2 condition, underscoring the necessity for accessible education and support. Resources such as education programs found in diabetes management pdf and support groups have been shown to significantly enhance an individual’s ability to manage their condition effectively.
Additionally, understanding the conversion from A1C to Estimated Average Glucose (eAG) is crucial for personalized care, helping individuals comprehend their long-term glucose levels and informing treatment adjustments. Conversion formulas and charts can facilitate this understanding, enabling patients to make informed decisions regarding their health. The integration of glucose management technology, including continuous glucose monitoring (CGM) and automated insulin delivery systems, is also recommended in the diabetes management pdf to improve glycemic control.
Moreover, evidence-based approaches, including cognitive behavioral therapy and sleep hygiene education, have been demonstrated to enhance sleep results and potentially support blood sugar control, complementing conventional education on the condition. As Dr. Jane Smith, a specialist in diabetes education, emphasizes,
‘Empowering individuals with knowledge and skills is crucial for effective control and enhanced health results.’
This perspective illustrates the evolving landscape of self-care education for managing blood sugar levels and its significant impact on patient outcomes.
Effective Strategies for Diabetes Management: Lifestyle and Medical Interventions
Effective oversight of type 2 diabetes necessitates a strategic blend of lifestyle changes and medical interventions, particularly through the lens of functional medicine. This personalized approach tailors strategies to individual health profiles, emphasizing the importance of comprehensive assessments and diagnostic tests to understand the root causes of the condition. Adopting a balanced diet that prioritizes whole grains, vegetables, and lean proteins is essential, alongside regular physical activity.
Personalized nutrition plans and stress management techniques are integral to this approach. Such lifestyle modifications are supported by findings from clinical studies, including the European Diabetes Prevention Study, which demonstrated an incidence rate of only 5% in participants who underwent lifestyle changes, compared to 11.1% in the control group. As Knowler WC noted, ‘In total, 34% reduction in lifestyle intervention group and 18% reduction in metformin group as compared to placebo control group,’ emphasizing the effectiveness of these interventions.
However, it is important to recognize the limitations of existing studies, particularly the absence of research from low-income countries and the predominance of studies from Asia, which may affect the generalizability of these findings. Furthermore, medical interventions should also be personalized to meet individual wellness needs, integrating conventional treatments with holistic practices. For instance, the DPP study highlighted a significant 34% reduction in the occurrence of the condition within the lifestyle intervention group after a decade, underscoring the long-term benefits of such changes.
In Iran, where approximately 5 million people are estimated to be affected by diabetes—a number expected to double by 2040—these strategies are particularly relevant. Regular consultations with healthcare providers are critical to tailor treatment plans effectively, ensuring that both lifestyle and medical strategies work synergistically to enhance glycemic control and minimize the risk of complications.
The Role of Healthcare Professionals in Diabetes Management
Healthcare professionals—including endocrinologists, educators for glucose regulation, dietitians, and mental health specialists—are essential to effective management of Type 2 condition. They offer customized care that enables individuals to eliminate insulin dependency and prevent gestational diabetes through education and tailored treatment plans designed around specific needs. Traditional treatment regimens can often be inconvenient and costly, leading many individuals to seek alternative solutions.
Evidence indicates that approximately 70.8% of individuals with Type 2 Diabetes exhibit systolic blood pressure levels of 140 mmHg or higher, underscoring the need for comprehensive care strategies. Significantly, GP consultations generally continue for just 15–20 minutes, whereas chronic healthcare providers allocate 30 to 60 minutes for each session, illustrating the depth of care provided in handling chronic conditions. Educators and dietitians play a critical role in equipping individuals with the knowledge necessary to understand their condition and the importance of adhering to personalized nutrition plans.
The urgency of efficient control of the condition is emphasized by the fact that the illness ranked as the eighth leading cause of death in the United States in 2021. Frequent consultations promote continuous assistance that motivates individuals to take control of their diabetes care. As noted by Carolyn J. Green, a web-based chronic illness coordination approach was pivotal in enhancing physician practices by systematically tracking care processes using evidence-based guidelines. This method demonstrates how systematic tracking and education can significantly enhance outcomes for individuals. The recent case study titled ‘Performance Measurement of Diabetes Management Care’ demonstrates that healthcare professionals’ effectiveness is evaluated based on the range of services provided, aligning with the National Basic Public Health Service Guideline.
This emphasizes the necessity for continuous assessment in diabetes management. Such comprehensive, team-based care is crucial for fostering informed decision-making and ultimately improving health outcomes for individuals living with Type 2 Diabetes. By opting for personalized consultations instead of generic diets, individuals can address their unique dietary needs more effectively.
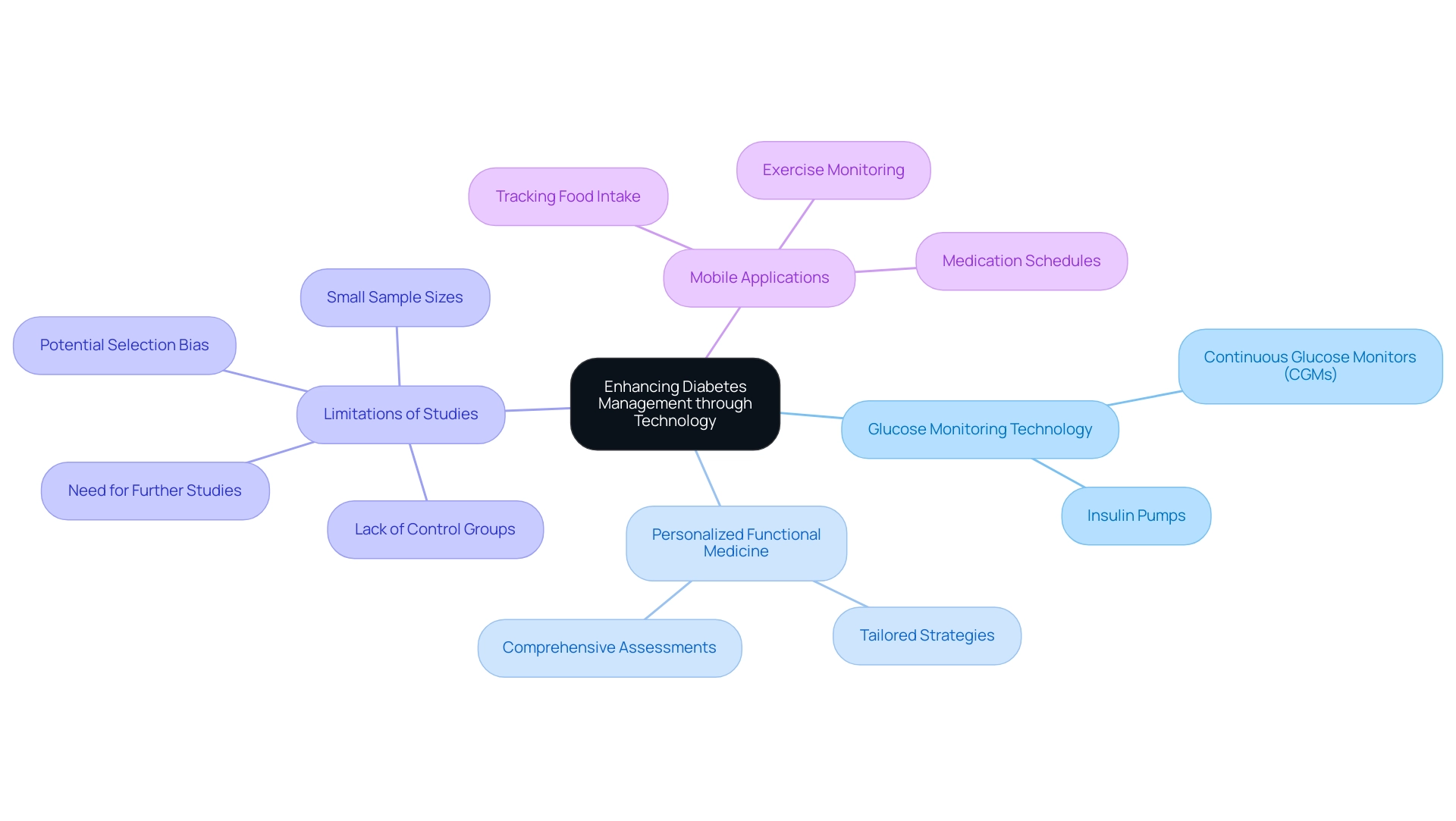
Monitoring and Technology: Enhancing Diabetes Management
Advancements in glucose monitoring technology, particularly the development of continuous glucose monitors (CGMs) and insulin pumps, have significantly transformed the oversight of the condition. These innovative tools offer individuals real-time data on their blood glucose levels, enabling immediate adjustments to their diet and medication regimens. For example, recent research shows that 16% of individuals with type 2 blood sugar disorders stopped using rapid-acting insulin after switching to CGM, highlighting the effect of this technology on medication oversight.
However, it’s essential to recognize the limitations of these studies, including small sample sizes and the lack of control groups, which may affect the generalizability of the findings. Furthermore, identifying populations with low CGM use is crucial for developing targeted interventions to enhance CGM uptake and management of the condition. Mobile applications complement these devices by assisting users in tracking food intake, exercise, and medication schedules, thus promoting a proactive approach to diabetes management.
Integrating these technological advancements with a personalized functional medicine approach, as advocated by Dr. Jason Shumard, allows individuals to manage their diabetes more effectively. This involves crafting tailored strategies that not only focus on monitoring but also address underlying health issues through comprehensive assessments and diagnostic tests, dietary needs, and lifestyle choices. This personalized approach helps avoid inconvenient and costly treatment regimens, enhancing overall client satisfaction.
The director of the UAB Multidisciplinary Comprehensive Diabetes Clinic, Dr. Fernando Ovalle, noted the potential of CGMs, stating, “Today I put one on a doctor who is not on insulin.” This reflects the broad applicability of CGMs in diverse groups. Overall, while the use of these technologies has been linked to enhanced glycemic control and increased satisfaction among individuals, further studies with extended follow-up are required to evaluate the long-term effectiveness of CGM systems and their connection with complications related to the condition.
Addressing Emotional and Psychological Needs in Diabetes Care
Living with this condition can significantly impact mental health, often resulting in increased feelings of anxiety, depression, and burnout among patients. Research indicates that symptoms of anxiety and depression can adversely affect health-related quality of life (HRQoL) over time, highlighting the need for healthcare professionals to recognize and address these emotional challenges. Alain K. Koyama, from the Centers for Disease Control and Prevention, emphasizes that,
Ongoing surveillance of diabetes and depression is essential to monitor changes at the local and state level.
Psychological counseling, support groups, and stress management techniques have been shown to be effective in mitigating these issues. Significantly, a longitudinal study titled “Longitudinal Associations in Diabetes Care” revealed important bi-directional pathways between mental well-being and HRQoL, suggesting that both anxiety and depression can negatively influence quality of life and vice versa. Furthermore, treatment with insulin-containing regimens has been associated with a lower risk for depression, with an adjusted odds ratio (AOR) of 0.49, reinforcing the importance of comprehensive care for blood sugar management.
However, it’s essential to acknowledge the limitations of these studies, such as potential biases in self-reported data and a short follow-up period of three months. Thus, promoting open dialogue regarding mental health not only assists individuals in feeling understood and supported but also encourages improved adherence to management plans, ultimately resulting in enhanced overall well-being. The prevalence of anxiety and depression in diabetes patients underscores the importance of integrating emotional support into comprehensive diabetes care.
Conclusion
Effective diabetes management is a multifaceted approach that hinges on self-care, education, and the integration of modern technology. By understanding the condition and actively participating in self-care practices—such as:
- Regular blood glucose monitoring
- Medication adherence
- Informed dietary choices
individuals can significantly improve their health outcomes. Success stories from programs like the 30-Day Diabetes Reset highlight the transformative potential of these strategies, demonstrating that empowered patients can achieve substantial health improvements.
Moreover, the collaboration between healthcare professionals and patients is crucial. Tailored treatment plans that incorporate lifestyle changes and medical interventions ensure that care is personalized and effective. The evidence underscores the importance of a comprehensive approach, blending functional medicine with ongoing support from a diverse healthcare team. This partnership not only enhances glycemic control but also addresses the emotional and psychological aspects of living with diabetes.
Technological advancements, such as continuous glucose monitors and mobile applications, further empower patients to take charge of their diabetes management. These tools provide real-time data and foster proactive decision-making, ultimately leading to better health outcomes. However, it remains essential to address the emotional challenges that accompany diabetes, as mental health significantly impacts overall well-being and adherence to treatment plans.
In summary, effective diabetes management requires a commitment to self-care, professional guidance, and the utilization of innovative technologies. By adopting a holistic strategy that encompasses both physical and emotional health, individuals can take control of their diabetes, improve their quality of life, and reduce the risk of complications. The journey towards better health is a collaborative effort, and with the right resources and support, managing diabetes can become an achievable goal.
Frequently Asked Questions
What is essential for effective diabetes management?
Effective diabetes management starts with a thorough understanding of the condition and the critical importance of self-care, which includes regularly monitoring blood glucose levels, adhering to prescribed medications, and making informed dietary choices.
How does education play a role in diabetes management?
Education empowers individuals to understand their diabetes management, recognize symptoms of hyperglycemia and hypoglycemia, and implement necessary lifestyle adjustments.
What are some success stories from Dr. Jason Shumard’s 30-Day Diabetes Reset Program?
Participants have reported significant improvements, such as substantial weight loss and reduced reliance on medications. For example, one individual lost 55 lbs and reduced their A1C from 9.1 to 5.7, while another reported increased energy and no longer needing medications.
Why is there a need for accessible education and support regarding diabetes?
Recent statistics show an increase in diagnoses of type 2 diabetes among children and adolescents, highlighting the necessity for accessible education and support resources to help manage the condition effectively.
What is the significance of understanding the conversion from A1C to Estimated Average Glucose (eAG)?
Understanding the conversion is crucial for personalized care, helping individuals comprehend their long-term glucose levels and informing treatment adjustments.
What technologies are recommended for improving glycemic control?
The integration of glucose management technology, including continuous glucose monitoring (CGM) and automated insulin delivery systems, is recommended to enhance glycemic control.
What evidence-based approaches can support diabetes management?
Evidence-based approaches such as cognitive behavioral therapy and sleep hygiene education have been shown to improve sleep outcomes and potentially support blood sugar control.
What is the role of lifestyle changes in managing type 2 diabetes?
Effective oversight of type 2 diabetes requires a strategic blend of lifestyle changes and medical interventions, including a balanced diet, regular physical activity, personalized nutrition plans, and stress management techniques.
What findings support the effectiveness of lifestyle interventions?
Clinical studies, such as the European Diabetes Prevention Study, demonstrated that participants who underwent lifestyle changes had a significantly lower incidence rate of diabetes compared to control groups.
Why is personalized treatment important in diabetes management?
Personalized treatment is crucial as it tailors medical interventions to meet individual wellness needs, integrating conventional treatments with holistic practices to enhance glycemic control and minimize complications.
List of Sources
- Foundations of Diabetes Management: Self-Care and Education
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10725800)
- National Diabetes Statistics Report (https://cdc.gov/diabetes/php/data-research)
- diabetesjournals.org (https://diabetesjournals.org/care/article/47/Supplement_1/S77/153949/5-Facilitating-Positive-Health-Behaviors-and-Well)
- Effective Strategies for Diabetes Management: Lifestyle and Medical Interventions
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC6893436)
- bmcendocrdisord.biomedcentral.com (https://bmcendocrdisord.biomedcentral.com/articles/10.1186/s12902-023-01445-9)
- thelancet.com (https://thelancet.com/journals/eclinm/article/PIIS2589-5370(22)00380-7/fulltext)
- The Role of Healthcare Professionals in Diabetes Management
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC7054922)
- National Diabetes Statistics Report (https://cdc.gov/diabetes/php/data-research)
- bmcprimcare.biomedcentral.com (https://bmcprimcare.biomedcentral.com/articles/10.1186/s12875-023-02136-z)
- Monitoring and Technology: Enhancing Diabetes Management
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10460137)
- diabetesjournals.org (https://diabetesjournals.org/clinical/article/42/3/388/154160/Patterns-and-Trends-in-Continuous-Glucose)
- uab.edu (https://uab.edu/reporter/patient-care/advances/item/10003-this-diabetes-technology-is-transforming-care-one-meal-at-a-time-expert-says)
- diabetesjournals.org (https://diabetesjournals.org/care/article/43/5/1146/35705/Effects-of-Continuous-Glucose-Monitoring-on)
- Addressing Emotional and Psychological Needs in Diabetes Care
- cdc.gov (https://cdc.gov/pcd/issues/2023/22_0407.htm)
- nature.com (https://nature.com/articles/s41598-020-57647-x)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S2667036422000085)